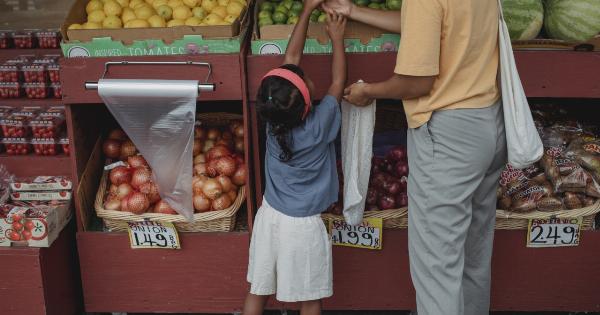Health insurance is essential for providing financial protection against costly medical treatments and procedures.
However, insurers may deny coverage for a treatment that a patient’s doctor has recommended, stating that it is not medically necessary. This may result in a significant financial burden on the patient, who has to pay for the treatment out-of-pocket.
In this article, we will discuss why insurers may decide that a treatment is not medically necessary, what to do if your doctor’s recommendation is denied, and how to appeal the decision.
What does it mean when insurers determine a treatment is not medically necessary?
Insurance companies have teams of medical professionals who review claims and determine whether a suggested treatment is “medically necessary.” Medically necessary treatments are those that are consistent with generally accepted medical practices, essential for diagnosing or treating a medical condition, and appropriate according to the standards of good medical care.
Insurance policies may generally cover only treatments that are considered medically necessary. When a treatment is not considered medically necessary, the insurance company has the right to deny coverage.
However, just because a treatment is not covered by an insurance policy does not necessarily mean it is not medically necessary.
Why do insurers deny coverage for medically necessary treatments?
Insurance companies may deny coverage for medically necessary treatments for a variety of reasons, including:.
- The treatment is considered experimental. Insurance companies may not cover new treatments or procedures until they are approved by the FDA or have been proven to be effective through appropriate studies.
- There is a less expensive alternative treatment. Insurance companies may deny coverage for a more expensive treatment if a less expensive alternative is available that would be just as effective.
- The treatment is not within the allowed coverage under the policy. Insurance policies may have limitations on coverage for certain treatments or procedures, or may exclude certain types of treatment altogether.
What should you do if your doctor’s recommended treatment is denied?
If your insurance company denies coverage for a treatment that your doctor has recommended, you have a few options:.
- Appeal the decision. If you believe that your doctor’s recommended treatment is medically necessary and should be covered by your insurance policy, you can appeal the decision. Each insurance company has its own appeals process, which you can find in your policy documents. Typically, you will need to provide additional documentation or information to support your appeal.
- Discuss alternative treatments with your doctor. Your doctor may be able to recommend alternative treatments that are covered by your insurance policy and would be just as effective as the recommended treatment.
- Pay for the treatment out-of-pocket. If your insurance company denies coverage for a recommended treatment and you cannot appeal or find an alternative treatment, you may choose to pay for the treatment out-of-pocket.
How to appeal a denied treatment?
When you file an appeal with your insurance company, you will need to provide documentation to support the medical necessity of the treatment your doctor has recommended.
This may include medical records, test results, and a letter of medical necessity from your doctor explaining why the treatment is necessary for your condition.
You can also contact your state’s insurance department to file a complaint or seek assistance in the appeals process.
The department can provide guidance on the appeals process and may be able to mediate the dispute between you and your insurance company if necessary.
Conclusion
Insurers may deny coverage for treatments deemed not medically necessary, but it is important to remember that doctors are the ones who determine the medical necessity of a treatment, not insurance companies.
If you believe that a recommended treatment is medically necessary and your insurance company denies coverage, you have options. However, it is essential to know your policy, understand the appeals process, and provide documentation to support your appeal.