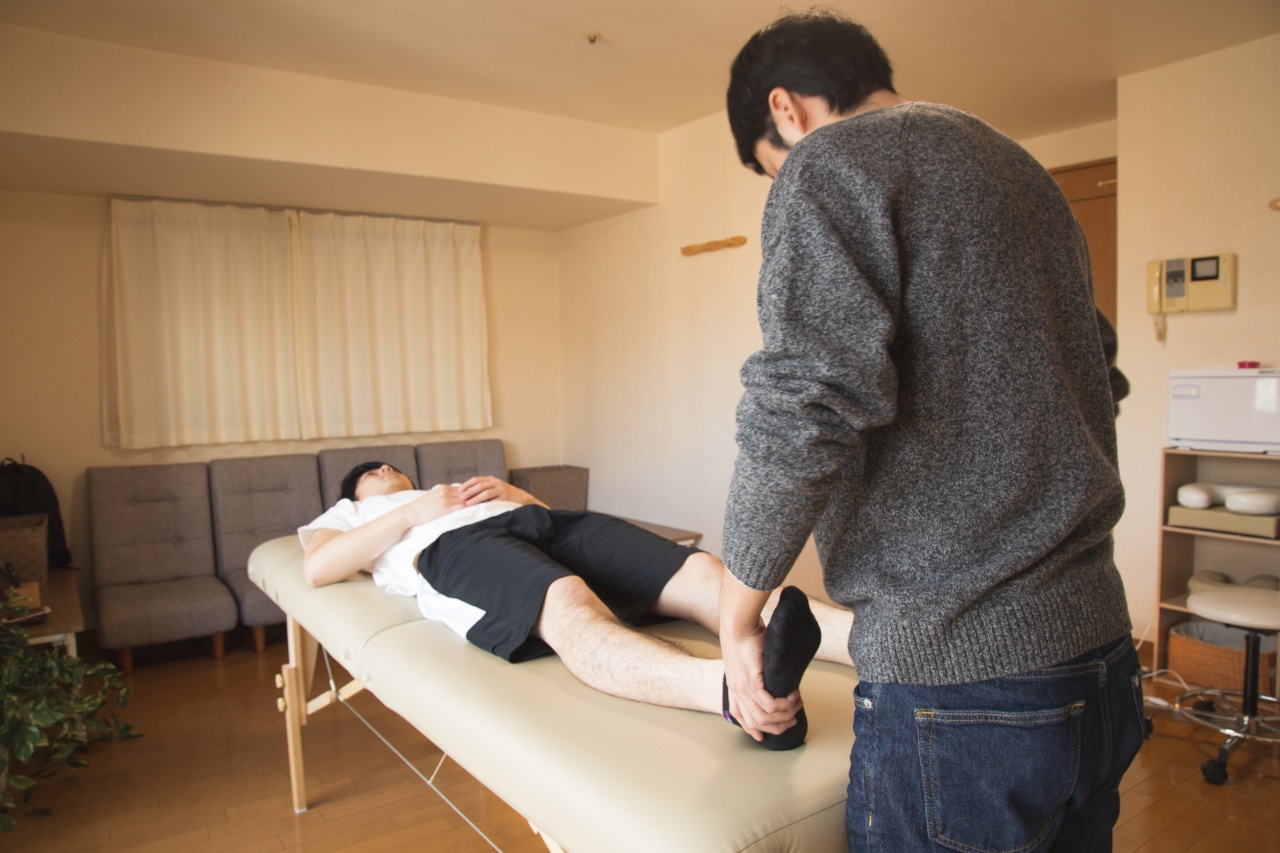
Occupational therapy and physiotherapy are two crucial healthcare services that help individuals regain their physical functionality and independence after injury, illness, or surgery.
These therapies involve specialized treatment plans, interventions, and exercises aimed at improving mobility, reducing pain, and enhancing overall well-being.
Although these therapies are deemed essential for many patients, it is unfortunate that some insurance companies do not fully cover these services.
This article aims to explore the reasons why certain occupational therapy and physiotherapy services may not be covered by insurance and shed light on the implications for patients, therapists, and healthcare systems.
1. Lack of insurance recognition and awareness
One major reason why certain occupational therapy and physiotherapy services may not be covered by insurance is the lack of recognition and awareness.
Insurance providers often have specific policies and guidelines dictating which therapies and services are eligible for coverage. However, due to limited understanding and awareness of the effectiveness and benefits of occupational therapy and physiotherapy, some insurers may not include them in their covered services.
2. Exclusion of specific conditions or treatments
Insurance coverage is often based on a predetermined list of covered conditions and treatments. Occupational therapy and physiotherapy services may not be explicitly mentioned or are only covered under certain conditions or treatments.
This exclusion can be frustrating for patients who require these therapies for rehabilitation purposes but are unable to access them due to insurance limitations.
3. Limited evidence-based research and documentation
Insurance companies heavily rely on evidence-based research and documentation to determine the effectiveness and necessity of a particular therapy or treatment.
Unfortunately, in some cases, there may be a lack of well-documented research showcasing the long-term benefits and cost-effectiveness of certain occupational therapy and physiotherapy interventions. This dearth of evidence can lead insurers to question the necessity of covering these services.
4. Cost considerations and budget constraints
The cost of healthcare services is a significant factor for insurance companies. Covering occupation therapy and physiotherapy services can be expensive, especially when considering the long duration of treatment required by some patients.
Insurers often face budget constraints and must make difficult decisions when it comes to coverage. Consequently, therapies that are perceived as costly may not receive full insurance coverage.
5. Varying insurance policies and plans
Insurance policies and plans can vary significantly between different providers and even between various plans offered by the same provider.
Some insurance plans explicitly exclude occupational therapy and physiotherapy services or limit coverage to a certain number of sessions or specific conditions. It is essential for patients to carefully review their insurance policies to understand the limitations and extent of coverage for these therapies.
6. Pre-existing condition clauses
Many insurance plans have pre-existing condition clauses that limit coverage for conditions or injuries that existed prior to obtaining insurance coverage.
This can pose a challenge for individuals who require occupational therapy or physiotherapy for pre-existing conditions, as these services may not be covered or may have limited coverage.
7. Lack of formalized guidelines and regulations
In some regions, there may be a lack of formalized guidelines and regulations defining the scope of coverage for occupational therapy and physiotherapy services.
This can create inconsistencies in insurance coverage, leading to confusion and limitations for patients seeking these therapies.
8. Insurance company profitability
Insurance companies are businesses aiming to maintain profitability. They carefully assess the cost and benefit of covering different healthcare services, including occupational therapy and physiotherapy.
If these therapies are perceived as yielding limited financial benefits or are deemed more costly compared to alternative interventions, insurance companies may choose to limit coverage or not cover them at all.
9. Overutilization concerns
Insurance companies worry about overutilization of healthcare services, which can lead to increased costs and potentially unnecessary treatments.
There may be concerns that if occupational therapy and physiotherapy services were fully covered, patients may seek excessive or prolonged therapy sessions. This concern about overutilization can influence insurance coverage policies for these therapies.
10. Lack of standardized reporting and outcome measures
Standardized reporting and outcome measures are critical in evaluating the effectiveness of occupational therapy and physiotherapy services.
However, the lack of consistent reporting and outcome measures across therapy practices can make it challenging for insurance companies to assess the success and impact of these therapies. This uncertainty can contribute to limited coverage for these services.
Conclusion
In conclusion, the limited coverage of occupational therapy and physiotherapy services by insurance companies can be attributed to various factors.
These include the lack of insurance recognition and awareness, exclusion of specific conditions or treatments, limited evidence-based research and documentation, cost considerations and budget constraints, varying insurance policies and plans, pre-existing condition clauses, the absence of formalized guidelines and regulations, insurance company profitability, overutilization concerns, and lack of standardized reporting and outcome measures. Addressing these issues requires collaborative efforts between healthcare professionals, insurers, policymakers, and patients to ensure that these vital therapies receive the coverage they deserve.