Osteoporosis is a condition that weakens the bones, making them fragile and more susceptible to fractures. It is often referred to as a “silent disease” because it progresses without any noticeable symptoms until a fracture occurs.
Bone mass measurement tests, also known as bone density tests or DXA scans, can help detect osteoporosis at an early stage and assess the risk of fractures. In this article, we will discuss the importance of these tests, who should consider getting tested, and what the results mean for your bone health.
What is Osteoporosis and Why is it a Concern?
Osteoporosis is a common bone disease that affects millions of people worldwide, particularly women after menopause. It occurs when the body loses too much bone, makes too little bone, or both.
As a result, the bones become weak and brittle, increasing the risk of fractures. Fractures caused by osteoporosis commonly occur in the hip, spine, and wrist, and can lead to severe pain, disability, and even death in some cases.
The alarming fact about osteoporosis is that it often goes undiagnosed until a fracture occurs. This is why it is crucial to detect it early and take preventive actions to minimize the risk of fractures.
Bone mass measurement tests play a vital role in identifying individuals with low bone density or osteoporosis, enabling early intervention and appropriate treatment.
What are Bone Mass Measurement Tests?
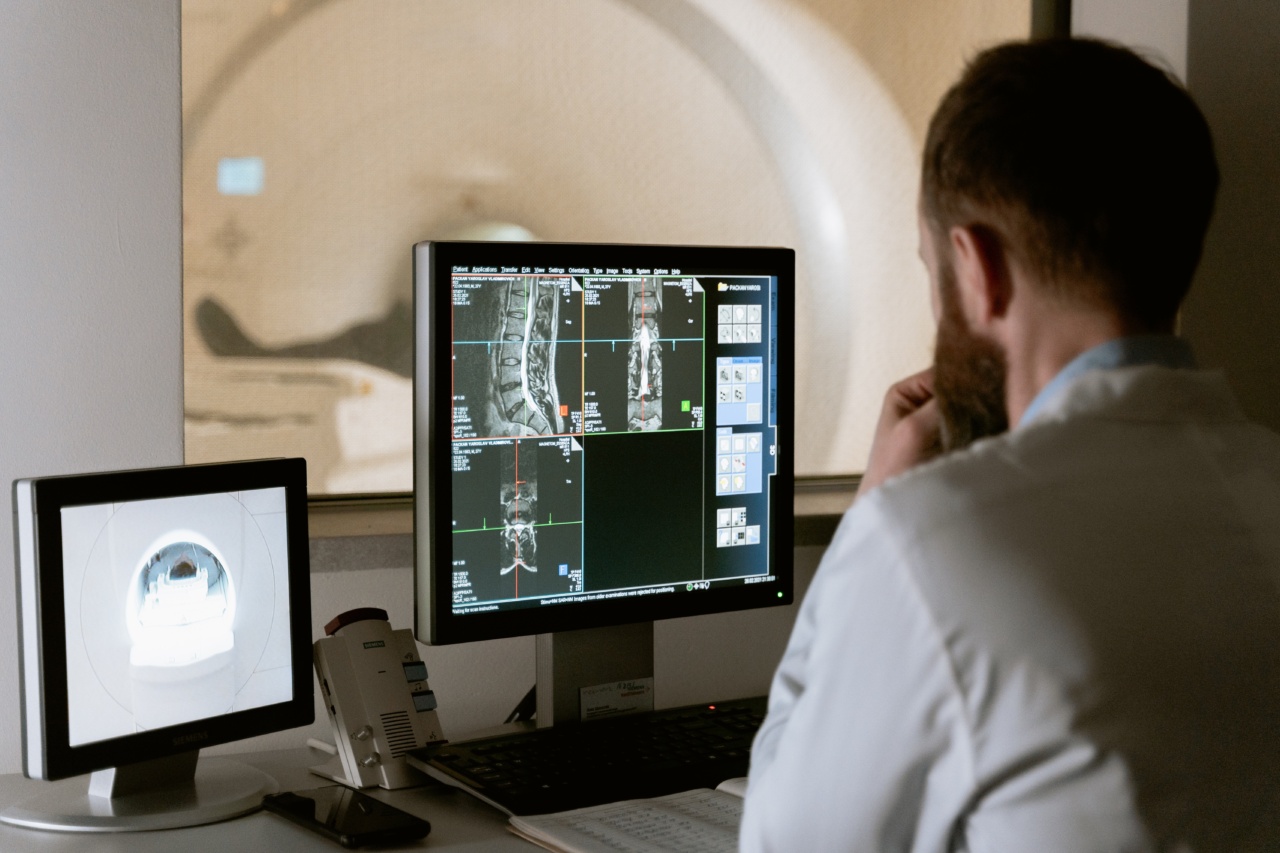
Bone mass measurement tests are non-invasive procedures that assess the density or strength of bones. The most common and accurate test used to diagnose osteoporosis is Dual-Energy X-ray Absorptiometry (DXA).
This test measures bone mineral density (BMD) at different sites of the body, commonly the hip and spine. It works by emitting two X-ray beams, each with a different energy level, which are absorbed by the bones. The amount of X-ray energy absorbed by the bones helps determine their mineral density.
The results of a DXA scan are usually reported as T-scores and Z-scores. The T-score compares an individual’s bone density to that of a healthy young adult of the same gender.
A T-score of -1 or above is considered normal, whereas a T-score between -1 and -2.5 indicates low bone density (osteopenia), and a T-score of -2.5 or below suggests osteoporosis. The Z-score compares an individual’s bone density to that of an average person of the same age, sex, and size.
Who Should Consider Getting a Bone Mass Measurement Test?
Not everyone needs to get a bone mass measurement test. However, certain factors increase the risk of osteoporosis and fracture, making it important to consider screening.
The following individuals are recommended to discuss the need for testing with their healthcare provider:.
- Postmenopausal women under the age of 65 who have one or more risk factors for osteoporosis.
- Postmenopausal women aged 65 or older, irrespective of their risk factors.
- Men aged 50 or older with risk factors for osteoporosis.
- Individuals who have experienced a fracture after the age of 50, as this could indicate underlying low bone density.
- Individuals with a medical condition or taking medications known to cause bone loss, such as rheumatoid arthritis, certain cancers, or long-term corticosteroid use.
- Individuals with a family history of osteoporosis or hip fractures.
It is essential to note that these guidelines are not absolute, and the decision to undergo a bone mass measurement test should be made after consulting with a healthcare professional, who will consider individual circumstances, risk factors, and medical history.
What Can the Results Tell You?
The results of a bone mass measurement test provide valuable information about your bone health. The T-score obtained from the DXA scan helps classify your bone density and assess the risk of fracture. Here’s what the T-score results indicate:.
- T-Score above -1: Your bone density is considered normal, and the risk of fractures is low.
- T-Score between -1 and -2.5: You have low bone density (osteopenia), which means you are at increased risk of fractures.
- T-Score of -2.5 or below: You have osteoporosis and are at a significant risk of fractures.
Based on the results, your healthcare provider will recommend appropriate further evaluation, lifestyle modifications, and treatment options.
Preventive measures may include changes in diet, increased physical activity, fall prevention strategies, and the use of medications to improve bone strength and reduce fracture risk.
How Often Should You Get Tested?
The frequency of bone mass measurement tests depends on various factors such as age, gender, previous test results, and the presence of specific risk factors.
It is generally recommended to repeat the test every 1-2 years to monitor changes in bone density over time. Your healthcare provider will determine the appropriate interval for repeat testing based on your individual circumstances.
Are There any Risks Associated with Bone Mass Measurement Tests?
Bone mass measurement tests, particularly DXA scans, are painless and involve minimal radiation exposure. The level of radiation exposure is significantly lower compared to most medical imaging tests.
The benefits of DXA scans in detecting osteoporosis and guiding treatment decisions far outweigh the potential risks.
However, it is important to inform your healthcare provider if you are pregnant or suspect you might be pregnant before undergoing a DXA scan, as radiation exposure should be minimized during pregnancy.
Conclusion
Osteoporosis is a serious condition that can have severe consequences if left undiagnosed and untreated. Bone mass measurement tests, such as DXA scans, are valuable tools for early detection and assessment of fracture risk.
If you belong to any of the high-risk groups or have risk factors for osteoporosis, consider discussing the need for a bone mass measurement test with your healthcare provider. Remember, prevention, early detection, and appropriate management can help maintain your bone health and reduce the risk of fractures.