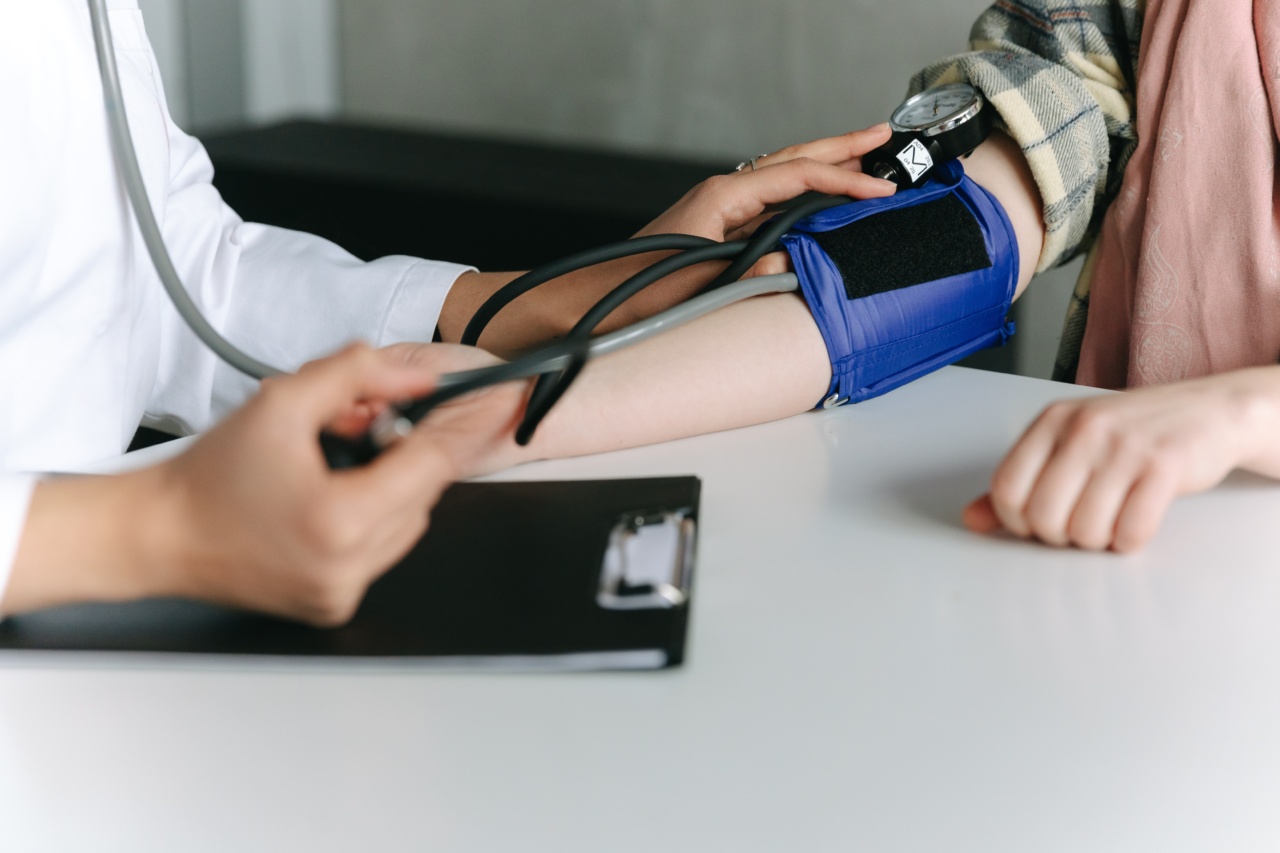
Hypertension, commonly known as high blood pressure, is a chronic medical condition that affects millions of people worldwide.
It is a condition in which the force of blood against the walls of your arteries is consistently too high, leading to potential health complications. While most cases of hypertension can be managed with lifestyle changes and medications, there are instances where blood pressure remains high despite treatment efforts.
In this article, we will explore the possible causes of hypertension that doesn’t go away and discuss potential solutions.
The Role of Lifestyle Factors
In many cases, lifestyle factors play a significant role in the development and management of hypertension. Poor diet, lack of physical activity, obesity, excessive alcohol consumption, and smoking are common contributors.
Making positive changes in these areas is often the first line of defense when dealing with hypertension. However, there are instances where even a healthy lifestyle isn’t enough to control blood pressure.
Underlying Medical Conditions
There are several underlying medical conditions that can cause chronic hypertension. Some of these conditions include:.
1. Kidney Problems
The kidneys play a crucial role in regulating blood pressure by controlling the fluid balance and electrolyte levels in the body.
Chronic kidney disease or kidney infections can impair their ability to function correctly, leading to hypertension that may not respond to conventional treatments.
2. Hormonal Imbalances
Hormones, such as aldosterone, renin, and thyroid hormones, play a vital role in maintaining blood pressure. When there is an imbalance in these hormones, it can lead to hypertension that is difficult to control.
Conditions like Cushing’s disease, primary aldosteronism, and an overactive thyroid can contribute to this problem.
3. Sleep Apnea
Sleep apnea is a sleep disorder characterized by interrupted breathing during sleep. It has been linked to hypertension, and studies have shown that controlling sleep apnea can lead to improvements in blood pressure.
However, for some individuals, even with adequate treatment for sleep apnea, their hypertension may persist.
4. Medications and Supplements
Certain medications and supplements can elevate blood pressure or interfere with antihypertensive medications, preventing them from effectively controlling hypertension.
Non-steroidal anti-inflammatory drugs (NSAIDs), oral contraceptives, decongestants, and some herbal supplements are known to have these effects.
5. Genetic Factors
Genetics also play a role in determining an individual’s susceptibility to hypertension. Some people may have genetic variations that make their blood pressure more difficult to manage.
Family history of hypertension and related cardiovascular conditions is an essential factor to consider when investigating the causes of chronic hypertension.
6. Stress and Anxiety
Stress and anxiety have a temporary effect on blood pressure. However, chronic stress can lead to long-term hypertension. It is linked to the release of stress hormones like cortisol, which can narrow blood vessels and raise blood pressure.
Managing stress through relaxation techniques and therapy can be beneficial but may not completely resolve hypertension in some individuals.
Treatment Approaches for Persistent Hypertension
If your hypertension isn’t responding to lifestyle modifications, medication, and other general interventions, it is crucial to consult a healthcare professional who can identify the underlying cause and suggest appropriate treatment approaches.
Possible strategies include:.
1. Additional Medications
Your doctor may prescribe additional medications or adjust the dosage to find the most effective combination for your specific condition. Different classes of antihypertensive drugs target different mechanisms in the body to lower blood pressure.
2. Targeted Therapy
If an underlying medical condition or hormonal imbalance is causing your hypertension, addressing that specific issue can help control blood pressure.
For example, treating kidney disease or adjusting thyroid hormone levels might lead to improvements in blood pressure.
3. Lifestyle Modifications
Continuing to prioritize lifestyle changes, such as adopting a balanced diet, increasing physical activity, losing weight if necessary, reducing alcohol consumption, quitting smoking, and managing stress, is essential even if these changes alone may not be sufficient to control blood pressure.
4. Monitoring and Record Keeping
Regular monitoring of blood pressure and keeping a record of readings can help healthcare professionals track patterns and determine the effectiveness of treatments.
This information is valuable in making evidence-based decisions regarding medication adjustments or additional interventions.
5. Specialist Referral
In some cases, your primary care physician may refer you to a hypertension specialist or a cardiologist who has expertise in managing complex hypertension cases.
These specialists can offer specialized testing, provide alternative treatment options, or conduct further investigations to identify the underlying cause of your persistent hypertension.
Conclusion
Hypertension that doesn’t go away can be frustrating and worrisome.
While lifestyle factors contribute significantly to the development of high blood pressure, there are numerous underlying medical conditions and genetic factors that may play a role in persistent hypertension. Identifying and treating these underlying causes is essential for effectively managing blood pressure and reducing the risk of associated complications.
By working closely with healthcare professionals and making necessary lifestyle changes, individuals with hypertension can strive for better control and overall cardiovascular health.